Posts
Press Release~There is Such a Thing as Being Too Thin…
FOR IMMEDIATE RELEASE Contact: Irina Strembitsky & Orchard Senior Living
Phone: (404) 775-0488
Email: marketing@orchardseniorliving.com
Press Release
There is Such a Thing as Being Too Thin…
Improved nutrition outcomes are within reach for those living with dementia and other chronic illnesses.
Tucker, Georgia, April 2nd, 2018- After a year of research, testing and development, Orchard Senior Living is prepared to unveil our custom created Nutrition Therapy Program specifically designed for those with dementia, as well as other chronic illnesses that often lead to malnutrition or undernutrition. We developed this program because the current nutrition therapy options available have failed our residents as well as many others in the community.
A popular saying says, “We are what we eat.” A good diet is vital to everyone’s health, well-being, and quality of life. A person needs carbohydrates, protein, fat, fiber, minerals, vitamins, electrolytes, and water to survive. Obtaining the correct balance and quantities of these nutrients is essential. Insufficient nutrition and hydration can lead to deterioration of overall health, including mental health, as well as weight loss, dehydration, dizziness, increased risk of falls, prolonged recovery after surgery, change of mood, frequent colds, reduced strength, reduced mobility, reduced communication abilities, difficulty keeping warm, infections, as well as prolonged healing. Cognitive deficits such as Dementia, have a direct effect on a person’s nutrition. Malnutrition or undernutrition may occur at any stage of dementia. It is important to detect it and try to remedy this as early as possible.
Did you know? Up to 45 per cent of people living with dementia experience clinically significant weight loss over one year, and up to half of people with moderate or severe dementia have an inadequate food and nutritional intake. Some experience very quick weight loss, dropping to a withering 70-90 lbs. in a span of several months. As dementia advances, it’s difficult to ensure that those living with dementia are eating and drinking enough. These challenges increase the risk for malnutrition and can worsen other health conditions a person may already have. There are numerous reasons for poor appetite to develop, including depression, communication problems, sensory impairments, change in taste and smell, pain, tiredness, medication side effects, physical inactivity, and constipation. Some people with dementia may lose their ability to concentrate, so they become distracted while eating and stop eating as a result. Other people may have trouble using utensils or raising a glass. It may also be challenging to bring the food from the plate to their mouth. Some people may need to be reminded to open their mouth to put food in it or even to chew. Another common problem in more severe dementia cases is dysphagia, which is difficulty swallowing. Dysphagia can lead to weight loss, malnutrition, or dehydration. Over time you may find that your loved one’s appetite declines or the taste of food doesn’t appeal to them. Sensory changes in sight and smell can impact their ability to enjoy food and mealtimes. Their likes and dislikes for food and drink may be quite dramatic and different from the ones they held for many years. They may also find it difficult to tell you what they want to eat.
Dementia and Alzheimer’s Disease are not the only chronic conditions that can cause malnutrition or undernutrition. Other chronic conditions can often impact a person’s nutrition. Many illnesses cause what is called disease-related malnutrition. Many people living with Parkinson’s disease, suffer from muscle weakness or tremors, which can make eating very challenging. Other diseases that often cause nutrition deficiencies are cancer, liver disease, COPD, and CHF to name a few.
In many of these cases, the malnutrition and undernutrition are severe and all conventional methods have failed. Orchard’s state of the art Nutrition Therapy Program offers hope for this group, a group that has not responded to traditional nutrition methods. Orchard has partnered with Gordon Foods and their team of experts and dieticians, as well as with dementia specialists to bring this revolutionary nutrition therapy to the community.
Join us on April 12th from 4 pm-6 pm as we unveil our Nutrition Therapy Program to area professionals who are interested in helping our community battle this difficult problem. Event attendees will be able to taste a variety of nutrition therapy options such as Cake a Boo, Sherberita, and Strawberry Smash. This event will be held at Orchard at Tucker, 2060 Idlewood Rd, Tucker GA 30084. For questions or to RSVP for the event please email marketing@orchardseniorliving.com.
Tips for Seniors (and their Families) on Downsizing Their Home
Sometimes seniors leave a big house to move to a senior community or assisted living. This new home may be more secure, healthier, and happier, but it’s also likely to be smaller.During this process, a family has two main tasks to focus on: helping their senior loved ones settle comfortably with valued possessions and preparing a house for sale. Downsizing with respect and practicality is important to both goals. Here are some transition to assisted living tips that you may find helpful during the process:
Cherished Possessions
It can be hard to separate possessions that truly matter from things that need to be let go. Be patient with anyone who lived in the house and feels attached to it, and expect difficult feelings as natural to the process. Just don’t let objects take priority over anyone’s well-being: the bottom line is that not everything can stay. If there’s not enough time to sort through everything with sensitivity, temporary storage may be the answer. Families can rent a unit or offer some home storage space so that no one feels stressed by any rush.
If there is time to sort through belongings, have seniors choose what goes to the new residence, what they would like distributed to family or friends, and what can be donated to charity. If children or grandchildren are just starting out in a new home themselves, seniors may be glad to contribute necessities they no longer need. Donations can also be satisfying when an item will help a stranger in need. Some charities will pick up goods and furniture by appointment.
It’s true that homes sometimes collect material things over decades, if homeowners don’t purge periodically. No family member should face exhaustion, or neglect their own family or livelihood, over each and every thing in a crowded house. Make sure the downsizing plan is appropriate for everyone. If the house is going on the market, sellers must declutter it of most contents and deep-clean. It must be staged to attract buyers. Seniors and their families need to commit to being understanding with each other, and also to getting the house sold efficiently.
There are tools that use local sales data to help you find the best time to sell in Atlanta. Statistics for 2014-2016 show that June and July are the best months for closing if you want the highest price possible on the home sale. Thus, listing in April or May, and having the house ready to show then, reaps sales about 7% over the yearly average. If your priority is to sell your house quickly, the data says you should aim for the same two months, since homes closing in June or July spend 1-2 weeks less on the market than those closing in other months of the year.
If you’re debating when to sell your house, find and ask an experienced local agent about the current state of the market and how you can maximize your home sale.
Written by Lin Nulman.
Can You Design a One Stop Shop Assisted Living Building?
Is it Possible to Design an Assisted Living Building to be a One Stop Shop?
The answer is yes, it is possible in theory, however the better question is, can a one stop shop design offer the best quality of life to most of the residents? I would venture to say no, because to design a community to fit your resident’s needs, you have a clear picture of who your resident will be, and design for their needs and preferences.
Who Lives in a One Stop Shop Design Building?
Many Assisted Living Communities attempt to be home, for a wide range of seniors, with a wide range of needs. This spectrum includes seniors with no to early mild dementia and no care needs, seniors that require ADL assistance ranging from standby to full assistance, as well as seniors in the late mild to late moderate dementia. Although these communities can market to a broader senior population, are all their residents getting the most of their community? Let’s break the spectrum into 4 groups of seniors and explore this further.
The Design Element of a One Stop Shop. Let’s Break It Down.
I am listing just a few of the preferences as well as needs, for each of the four groups, that a one stop shop building will need to accommodate.
Group 1 (independent senior that still drives some)
- Large floor plans, full kitchens (this group has no care costs to incur now)
- Multiple Dining Venues such as a bistro where you can get a sandwich (so they can come and go without missing a meal)
- Flexible Dining Times
- A Bar for Happy Hour
- Computer Classes
- Lots of Exercise Classes such as dancing and yoga, an Exercise Facility with exercise bikes
- Lots of different community amenities throughout- completely fine with a multi-story building, if it means more amenities
Group 2 (needs stand by ADL assistance)
- Less expensive smaller floor plans options (this group is incurring some care costs)
- Transportation offered by the community
- Exercise Classes such as chair exercises
- Multiple Dining Venues
- Amenities and Activities near their own living quarters
Group 3 (Seniors who need hands on ADL assistance)
- Less expensive smaller floor plans options (this group incurring the most care costs)
- Visiting medical professionals (limited mobility makes traveling difficult)
- Amenities very near to living quarters, as well as mobile amenities that can come to them
- Amenity areas they can use- this group can no longer enjoy an exercise bike, or a pool
Group 4 (Senior with late Mild-Moderate Dementia)
- Smaller floor plans to minimize confusion. Also incurring care costs at this level
- Set meal times in one place (we know structure is key to those with dementia)
- This one dining area should be fairly close to living quarters to minimize confusion
- Dementia friendly amenity areas such as a multi-purpose activity room (computer lab or a library are no longer an important amenity for many of these residents. Many of these residents are no longer able to drink so a bar is not important)
- Visiting medical professionals
- Smaller building design to lessen the confusion. (this group can no longer safely navigate a large building and find spread out amenity areas)
Is There Some Overlap with Needs and Preferences between Some of the Groups?
Although some of the needs and preference to overlap, there becomes a point that the preference of one group of seniors are the opposite of the preferences/needs of another group of seniors. Group 1 wants active, spread out amenities, in and outside the community. They want to do these activities in amenity areas through out the building. Group 2’s preferences do somewhat overlap with group 1. However, when you get to group 3 and 4, you notice no overlapping, but on the contrary conflicting needs and preferences. Another area where needs and preferences come to a head for the 4 groups is dining. Group 1 wants flexible dining times and multiple venues. Group 2 may also use these, but when you get to group 3, who is not able to get to these venues without assistance that preference diminishes. In many cases group 3 needs assistance with dining, such as making sure their foods are cut up, salad dressing is open, so a grab and go bistro is no longer a needed amenity. When you get to group 4, you notice a conflicting need with groups 1 and 2. Group 4 likes to eat at the same time, in the same place, with the same people for the most part. Also notice that the amenity preferences decrease as the care needs increase. Group 1 are the most active seniors, who also have the most amenity preferences.
The Take Away..
There are many areas where design needs and preferences overlap for some groups. They overlap for groups with similar physical and cognitive deficits. Group 1 had some similar preferences as group 2, but very few if any of the same preferences of group 3 and 4. Also once you got to Group 3 and 4, some of the preferences turn into needs due to physical and cognitive deficits.
One building can be designed for a spectrum of needs, but when that spectrum gets too large, some group will be left out from enjoying the entire community. Although it is easier to lease up a building with a larger pool of prospects, it is very difficult to cost effectively design a space that meets such a large spectrum of needs. The design element of a one stop shop is difficult to manage, although this element is a piece of cake compared to the care and engagement piece. It is almost impossible to provide care and engagement in a one stop shop community, and to do it well for everyone.
Visit http://stage-osl.daveminotti.com/category/blog/ to view future posts about providing care and engage ment in a one stop shop building.
ment in a one stop shop building.
The Need for Dementia Sensitive Primary Care
What was the Inspiration behind this post?
Last week I had a doctor’s appointment with my primary care doctor. It was a 3 pm appointment. Here it was almost 4 pm and I was just getting called. When my doctor saw me, she immediately apologized and told me the reason for the delay. She said that today many of her patients had dementia, and those appointments take longer than the other appointments, yet they are scheduled for the same amount of time. My doctor knows I work in senior living, so she felt comfortable telling me her feedback of her experience with dementia patients. My Doctor told me that she spends a large part of the appointment counseling her dementia patients and their families. She also told me, the most frustrating part of her appointments with those with dementia, is explaining to them, that there is little she can do medically to alleviate the symptoms caused by dementia. She said many family members for instance notice their loved one with dementia has suddenly lost weight, and they want a prescription to combat that. She then has to give them the disappointing news that weight loss caused by dementia is a comprehensive symptom and can’t be fixed over night with a prescription. Needless to say, she was very excited to hear about Orchard’s Brand New 4 Tier Nutrition Therapy Program coming in 2018. For more information about Nutrition Therapy for Dementia please visit: http://stage-osl.daveminotti.com/final-stages-of-nutrition-therapy-development-for-dementia-residents/, as well as http://stage-osl.daveminotti.com/nutrition-therapy-at-each-level-of-dementia-care/
What Does Dementia Sensitive Primary Care Mean?
Dementia Sensitive Primary Care, are primary care services that are provided solely to individuals living with dementia. These services are provided by professionals that specialize in dementia, and in many cases only treat those with dementia. This type of care can be provided in a clinic or by a mobile service, by a medical professional ranging from a Nurse Practitioner to a Doctor. This clinic and or professional is designed to replace a person’s primary care provider that they had prior to the dementia.
What is an Example of Dementia Sensitive Primary Care Center?
The Integrated Memory Care Clinic, located in Atlanta, is a nationally-recognized patient-centered clinic that provides primary care for someone living with dementia. The clinic provides a variety of services to meet the challenging needs of those living with dementia. Whether the patient living with dementia has a cold, needs a vaccine, or has a change in behavior, the clinic can help. Dementia and other chronic conditions are managed exclusively by nurse practitioners who collaborate with geriatricians and neurologists on the team. The nurse practitioners have advanced training and specializations in dementia, geriatrics, and palliative care. A clinical social worker is also a vital member of the team. I personally know people that are patients at The Integrated Memory Care Clinic, and I know some of the professionals that manage it. I can say this clinic does an absolutely amazing job, and I would recommend it to anyone who is looking for Dementia Sensitive Primary Care.
Can Dementia Sensitive Primary Care be done outside of a clinic?
The answer is yes. I personally work with several medical groups that provide concierge dementia sensitive care in a person’s home. They can go to someone’s home or to their community. The group I work with closest has a team of professionals that provide the care. Their team is made up of a Geriatric Psychiatrist, a Nurse Practitioner and a Doctor trained in dementia care, as well as an Occupational and Speech Therapist. These professionals work as a team to define the patient’s cognitive, functional and behavioral profile, and create a care plan to manage their care. The extent to which each specific professional sees the patient depends on the patient’s needs and their profile. These services are offered in a person’s home, and at the Orchard, or another community.
Why do we need Dementia Sensitive Primary Care for those with Dementia?
Currently, 50-90% of all dementia gets misdiagnosed or gets missed all together until a crisis happens. Even if Primary Care Professionals start to more accurately recognize dementia, the quality of management of the disease after the diagnosis is usually sub optimal. Even if a PCP can diagnose dementia, in many cases they do not have a plan for follow up management. After dementia is diagnosed, there needs to be a plan of care set up to address potentially starting dementia-specific drug treatment to slow the decline, assessment and management of Behavioral and Psychological Symptoms of Dementia (BPSD), safety issues in and out of the home, side effects of psychotropic drugs, as well as the stress of family care givers. Most Primary Care Professionals today are not equipped to provide follow up dementia care. These PCPs are missing the coordination of primary healthcare partners, as well as the implementation of support for both people with dementia and their caregivers. Hopefully in the next few years, more Integrated Memory Care Clinics will spring up, and more people with dementia will receive the Dementia Sensitive Primary Care they need.
as well as the implementation of support for both people with dementia and their caregivers. Hopefully in the next few years, more Integrated Memory Care Clinics will spring up, and more people with dementia will receive the Dementia Sensitive Primary Care they need.
Are Patients with Dementia Smarter than their Primary Care Practitioners?
Are Patients with Dementia Smarter than their Primary Care Practitioners?
The answer is not necessarily, however patients with dementia work much harder to mask and hide their dementia from the PCP, than their PCP works to diagnose their patients’ dementia.
How Has the Role of a Primary Care Practitioner Evolved?
Due to the increasing numbers of people living with Dementia and Alzheimer’s Disease, primary care practitioners, are seeing their patient loads be filled with more and more dementia patients. Primary Care Practitioners are usually the first health professionals that either patients or their families contact if concerned about memory decline. However only 60% of the people who meet the diagnostic criteria receive a formal diagnosis of dementia. Failure/Misdiagnosis rates have been estimated between 50% and 80% for moderate-to-severe dementia and up to 90% for mild cases. PCPs are usually the ones who have a long relationship with patients as well as their families, so patients and their families usually turn to the PCPs for sensitive matters such as memory loss or other signs of dementia.
Why is there such as high rate of Failure and Misdiagnosis? The Too Simple of an Answer…
Most primary care practitioners do not specialize in dementia and therefore symptoms get missed. Most PCPs rush through the appointments and do not take the time to notice dementia symptoms. Another too simple of an answer, PCPs treat dementia like they do other chronic illnesses by prescribing medications and sending the patient home. Although there is some truth in all these answers, the real answer is much more complicated.
The Real-Life Reason there such as high rate of Failure and Misdiagnosis?
Although there is some truth in the simple answers, they don’t paint the entire picture. Understanding and diagnosing dementia takes more than just being familiar with the typical dementia symptoms and being able to recognize them. There are many symptoms of Alzheimer’s and Dementia that a person exhibits before significant memory loss. Many people and their families discount these symptoms as just general senility or some other problem. These symptoms include personality changes. A warm, friendly person may turn into a bit of a grouch, at first occasionally, and then increasingly. They may start neglecting some of their grooming habits slowly. A person developing dementia may start telling inappropriate jokes in wrong settings. Another symptom is developing a problem with executive functions, such as difficulty with familiar, tasks such as cooking. A person will start having difficulty doing something that involves multiple steps, or following instructions. Word retrieval and getting out the right words can become a problem, and it may be a while before friends and family notice the more common communication problem of repeating stories or questions. Problems with depth perception or visual-spatial coordination can also precede memory problems. Usually these difficulties get blamed on vision problems and not dementia. Apathy and social withdrawal are also common with dementia. All these symptoms often precede memory loss, yet can easily be justified as being caused by something else other than dementia. Until a certain point, these symptoms do not significantly impact a person’s life, and therefore get ignored, and ultimately dementia is not diagnosed. One of the largest culprits of a missed diagnosis is masking by the person that has dementia. People with dementia usually notice something is wrong and they do everything they can to hide it. So even if a PCP asks their patient about one of the above symptoms, the patient easily comes up with a pliable excuse, such as they are tired and don’t  want to do a hobby, the weather is bad, they are stressed, they need new glasses, they are not sleeping well and therefore their mind is foggy, and on and on. If a person with dementia misses their appointment, they are likely to blame it on the doctor’s office, or someone else, and even avoid making future appointments all together, due to the fear of missing the next appointment. It is very difficult, if not impossible for a PCP that treats a spectrum of patients including those with dementia and without to be able to pick up on these subtle symptoms. They are not focusing on these subtle symptoms, and because many of their patients do not have dementia, dementia and its symptoms are not in the fore front.
want to do a hobby, the weather is bad, they are stressed, they need new glasses, they are not sleeping well and therefore their mind is foggy, and on and on. If a person with dementia misses their appointment, they are likely to blame it on the doctor’s office, or someone else, and even avoid making future appointments all together, due to the fear of missing the next appointment. It is very difficult, if not impossible for a PCP that treats a spectrum of patients including those with dementia and without to be able to pick up on these subtle symptoms. They are not focusing on these subtle symptoms, and because many of their patients do not have dementia, dementia and its symptoms are not in the fore front.
Why We Rarely See a Person with Mild Dementia Move to Assisted Living?
Since upwards to 90% of people with mild dementia get misdiagnosed or missed, most people do not realize something is wrong until there are blatant symptoms that usually harm a person in some way. Most people do not notice or get alarmed with a few missed medication doses, until a person either takes to many pills, or takes too few, gets dizzy, and falls. Even in those cases, they go to the hospital and the fall is at the forefront, and not the dementia that caused a person to forget their medications and fall. Rarely do families notice that their loved one is not eating, until there is a significant and visual weight loss. Families usually do not notice that their loved one is neglecting their grooming until they look obviously disheveled. They don’t notice personality changes, until something out of character and usually embarrassing occurs in public, very often in church. Most people with dementia improve their masking abilities over time, and their dementia is not addressed until they are not able to mask anymore, which is usually in the Early Moderate Stage of Dementia. By that time in many cases, substantial damage has been done, such as substantial weight loss, a broken bone due to an avoidable fall, and so much more.
The Take Away….
The solution to the huge percentages of failure/misdiagnosis of dementia, and the damage caused by these misses, is multi-faceted. There is a need for Comprehensive Dementia Education, Dementia Sensitive Primary Care Clinics and Doctors, and Cognitive Care Communities specializing in all levels of dementia from Mild to Severe. To find out more about the importance of a cognitive care community visit; http://orchardseniorliving.com/the-importance-of-a-cognitive-care-community-for-dementia-care/.
The next several posts will detail ideas and solutions to combating dementia caused crisis, and decrease the failure/misdiagnosis rates. Visit http://stage-osl.daveminotti.com/category/blog/
Dementia, I Will Give You My Memory, If You Leave Me My Personality
What Does Dementia Mean to the Average Person?
Dementia is a general decline in cognitive ability severe enough to interfere with daily life. Memory loss is one example. Dementia is not a specific disease. Dementia is a term that describes a wide range of symptoms associated with a decline in memory and other thinking skills severe enough to reduce a person’s ability to perform everyday activities. People with dementia often have problems with short-term memory recall, keeping track of a wallet or other possessions, paying bills, planning and preparing meals, remembering appointments or traveling out of the neighborhood. Dementia is progressive, as symptoms start out slowly and gradually get worse. As Dementia progresses, individuals notice increased memory loss, mental decline, confusion especially in the evening hours, disorientation, inability to speak or understand language, making things up, mental confusion, or inability to recognize common things.
What Does Dementia Mean to Those of Us Who See it Every Day?
Although the above examples of dementia symptoms are true, and do indeed interfere with a person’s everyday life, they are not a full picture of dementia symptoms. When dementia steals memory, language, thinking and reasoning, these new deficits are referred to as “cognitive deficits” of the disease. The term “behavioral and psychiatric symptoms” describes a large group of additional, and in my opinion most devastating, symptoms that occur to at least some degree in many individuals with dementia. In early stages of dementia, many experience personality changes such as irritability, apathy, anxiety or depression. In later stages, many experience sleep disturbances, mixing up their days and nights, agitation such as physical or verbal outbursts, combativeness, combativeness while getting care, refusal to get care, general emotional distress, restlessness, continuous pacing, shredding paper or tissues, yelling for no apparent reasons, delusions, paranoia, misperceptions, or hallucinations.
Real Life Example of a Behavioral Change.
Linda is 87 in the moderate stage of dementia. She retired as a Vice President of a company. Her family told me that she was known for her business acumen and immaculate appearance. Her outfits were always perfectly put together, her makeup and hair flawless. Today, due to the dementia, it is a struggle to get Linda to take a shower, comb her hair, or get any grooming what so ever. She refuses to wear makeup and will very rarely agree to get her hair done. She refuses manicures and pedicures that she used to get weekly for over 40 years. It is extremely painful for her family to watch Linda, who was always so well put together, now refuse to get her hair done, and be combative when any grooming is attempted. Unfortunately, this type of a personality change is common to those with dementia. Dementia has stripped Linda of her desire to look nice and be well groomed. In a year’s time, dementia has changed grooming habits Linda had for over 40 years.
Real Life Example #2
Lynn is 84 in the moderate stage of dementia. She worked as party planner before she retired. She was always very social and the life of the party. Lynn remained social into the mild stages of dementia. During the tail end of the mild stage, Lynn was still social, however when she would be around others they would ask her questions about her family and herself that she had trouble answering due to her dementia. Each time Lynn was not able to answer a question, she would leave the social or the event immediately. Shortly after, Lynn refused to participate in any of the hobbies and socials she enjoyed her whole life. This is another common example of dementia changing a person’s personality, and converting a social butterfly into a reclusive butterfly.
Lynn was reclusive and isolated for several months. Finally, her family decided to move her to the Orchard at Tucker, a community that specializes in cognitive care and engagement for those with cognitive deficits. Lynn’s family provided the Orchard with a detailed profile as well as her history and the Orchard engagement team came up with a detailed plan to combat Lynn’s new reclusive personality. The engagement team took all the information they were given, and they were able to create an Enabling Environment for Lynn. To learn more about enabling an environment see http://stage-osl.daveminotti.com/creating-an-enabling-environment-is-key-to-providing-dementia-care/)
With the creation of a new enabling environment, Lynn slowly started to participate in some activities. Although the Orchard engagement team did several things to modify her environment, one such modification was surrounding Lynn with other residents that were on her cognitive level. They also made sure that all team members were aware of Lynn’s history and her strong desire to mask her dementia. When everyone was aware of Lynn’s dementia, and the other resident around her also had dementia, no one asked Lynn any difficult questions, and her dementia never stood out to others. This one environmental change alone led to Lynn participating in activities daily, although never to the extent she used to participate prior to the dementia. Environmental modifications are very helpful, but they can never make up for all the damage caused by dementia. In Lynn’s case, her personality change could have been minimized if an enabling environment was created sooner. I believe Lynn’s personality change was so significant, so quickly, at least in part due to Lynn losing her self-esteem by not being able to answer the questions asked, and her struggle to hide her dementia from those that were noticing. This is a prime example of a personality change that dementia caused, that could have been lessened by an earlier intervention.
The Take Away..
I have spoken with so many loved ones of those with dementia, and they have all agreed, that the behavioral changes caused by Dementia that are hardest on their loved one, as well as the entire family. Losing your memory is nothing compared to becoming a different person. Also, it is the behavioral changes caused by dementia that impact one’s life, much more negatively than memory loss. It is much easier to compensate for a person’s memory loss than to compensate for extreme anxiety, paranoia, combativeness, or refusal to get care. These behavior symptoms are rarely talked about. When you ask the average person what dementia means, they will say dementia causes memory loss. Most people do not realize how many other terribly negative symptoms are caused by dementia. They don’t realize that if dementia just caused memory loss, most people with dementia would have a much better quality of life. Most people don’t understand the devastation dementia causes. Dementia causes comprehensive memory loss, not just memory loss of what happened yesterday, or what time it is, but in many cases the loss of one’s personality. Very rarely are the personality changes positive. Almost always these behavioral personality changes negatively impact a person’s quality of life. These changes often create a completely different person, often unrecognizable to friends and family. As dementia progresses, these changes happen quickly and become more and more noticeable. It is important to understand that they are still the same person inside. They have not changed on the inside, the way they now communicate with the outside world has changed. Dementia causes a person to have a battle, both internal and external, a battle for who they were, and how they were ones perceived.
Elevated Emotions Even Without Memory while Living with Dementia
Which last longer for those with Dementia or Alzheimer’s Disease? Memories or Emotion?
Have you seen long lasting emotions in a loved one with Dementia or Alzheimer’s after the memory causing the feelings have faded? I have on many occasions. Although I have seen it live on so many occasions, there is now science behind it. It’s no surprise that people with Alzheimer’ s have trouble recalling memories. It is, after all, the hallmark symptom of the disease. However, a new study has found that events can have a longer term and profound effect on how they feel even if they do not remember the particular event.
s have trouble recalling memories. It is, after all, the hallmark symptom of the disease. However, a new study has found that events can have a longer term and profound effect on how they feel even if they do not remember the particular event.
The Study..
A new University of Iowa study further supports an inescapable message: caregivers have a profound influence—good or bad—on the emotional state of individuals with Alzheimer’s disease. They may not remember a recent visit by a loved one or having been neglected by a loved one, but those actions can have a lasting impact on how they feel. University of Iowa researchers also showed individuals with Alzheimer’s disease clips of sad and happy movies. The patients experienced sustained states of sadness and happiness despite not being able to remember the movies.
The Emotional Life of those with Dementia and Alzheimer’s Disease….
These studies confirm that the emotional life of those with dementia and Alzheimer’s disease last far beyond the tangible memory of an event, regardless if the event was good or bad. “This confirms that the emotional life of an Alzheimer’s patient is alive and well,” says lead author Edmarie Guzmán-Vélez, a doctoral student in clinical psychology, a Dean’s Graduate Research Fellow, and a National Science Foundation Graduate Research Fellow.
The Take Away…
Despite the considerable amount of research aimed at finding new treatments for Alzheimer’s, no drug has succeeded at either preventing or substantially influencing the disease’s progression. Against this foreboding backdrop, the results of this study highlight the need to implement new care giving techniques and care models aimed at improving the well-being and minimizing the suffering for the millions of individuals afflicted with Alzheimer’s. These studies prove that traditional thinking about the emotional life of someone with Dementia and Alzheimer’s Disease is lacking immensely. Traditional thinking still tries to convince people that if they don’t remember it does not matter. At the Orchard at Tucker, we feel it Not Only Matters, but it Matters More. Although these studies are wonderful, we see the importance of emotion based care each and everyday by watching our residents.
The Biggest Misconception about the Dementia Brain in Dementia Care
Why is our brain so important?
The brain is the most important organ in the human body. It controls and coordinates actions and reactions, allows us to think and feel, and enables us to have memories and feelings. Furthermore the brain runs everything. It is the guiding, maintenance, and managing system for hundreds of a human beings needed abilities.
When does dementia occur? The quick answer…
Dementia occurs when the brain is damaged by disease. Sometimes it is one part of the brain, sometimes it is multiple parts.
To understand dementia, we must first understand the brain…
The brain can be divided into different parts: the brain stem and cerebellum, the limbic system, and the cerebral hemispheres. Each part has different functions.
Brain stem and cerebellum…
The brain stem is at the base of the brain. It controls basic bodily functions such as heartbeat and breathing. The cerebellum
controls balance and posture. Breathing and staying upright are things that we normally do automatically.
The limbic system…
The limbic system is deep inside the brain. It links the brain stem and the cerebral hemispheres. The limbic system includes structures with key roles in memory (the hippocampus) and emotions (the amygdala). The limbic system is the first part of the brain to develop and is sometim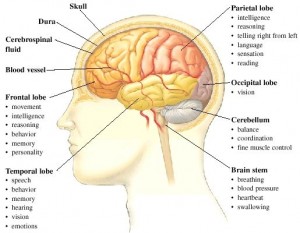 es referred to as our “primal brain” and manages many of our survival reflexes. It includes the amygdala which is in charge of the “flight, fright, fight response.
es referred to as our “primal brain” and manages many of our survival reflexes. It includes the amygdala which is in charge of the “flight, fright, fight response.
Cerebral hemispheres…
The tissue that makes up three-quarters of the brain is called the cerebrum. It is responsible for consciousness, memory, reasoning, language and social skills. A deep groove that runs from the front to the back of the cerebrum divides it into left and right halves: the two cerebral hemispheres.
The left and right cerebral hemispheres have different functions. For example, language is usually dealt with mainly by the left hemisphere. In contrast, awareness of where things are around us is usually dealt with mainly by the right hemisphere.
The lobes….
The four lobes are: occipital, temporal, parietal and frontal lobes. Each lobe does different things, though they also work closely together.The lobes are responsible for our senses. There are 5 ways human beings take in information (data) about the world through their nervous system.. What you see, hear, touch/feel, smell, and taste.
you see, hear, touch/feel, smell, and taste.
The lobes are some of the first areas effected by Dementia..
Dementia diseases often impact abilities in the occipital lobe of the brain which affect a person’s visual field. Dementia commonly affect the temporal lobes asymmetrically; typically attacking left temporal lobes before the right. This means more loss in language stored on the left, and more preserved skills for much longer. In dementia, different forms of damage to the lobes in the brain can cause someone to become either over-emotional or lacking in feelings. This is one of the reasons that a person with dementia exhibits changes in behavior along with memory loss. Sometimes the changes in behavior may be more pronounced than the memory loss. In these cases, many times dementia gets misdiagnosed since common thinking is, that dementia causes just memory loss.
What is the biggest misconception about the dementia brain and those with dementia?
Emotional memory is stored in the hippocampal area and is commonly a preserved skill. Persons living with dementia may not remember the details of what happened, but will almost always remember how an experience made them feel. Traditional thinking is if someone does not remember what they did specifically shortly after they did it, their day has less relevance, their life should be less purposeful. This is the biggest misconception in traditional dementia care. Those with dementia may get to a point that they don’t remember going to a great concert the next day, or helping to bake and delivering cookies to a police department, but they remember till almost the very end how much they enjoyed the concert, and how good they felt delivering those cookies over to those officers.
The Take Away…..
Orchard Senior Living is determined to bring a new type of dementia care to those inflicted with dementia. It is an engagement focused cognitive care model, where we focus on activities that will be stored in our residents’ emotional memories which they will have with them till they take their last breath.
Nutrition Assessment is a Part of Dementia & Alzheimer’s Care
Determining if your loved one needs additional nutrition care or nutrition therapy starts with a nutrition assessment.
What is Nutrition Assessment?
Nutrition assessment is a process that nutritionist or dietitian uses to evaluate your nutrition level and determining your current nutrition needs. Your nutrition level ranges from great to extremely deficient. The first step is to determine your individual nutrition needs for optimal health. This step includes knowing a thorough history of your diet, lifestyle, medical, chronic conditions. The second step is the evaluation of your nutrition status, calorie, protein and nutrient needs, adequacy of your diet, possible deficiencies or food intolerance(s), need for further testing, recommendations for diet and lifestyle changes and supplements.
Your Nutrition Assessment looks at all these areas:
- Diet history
- History of Weight Loss
- Recent illnesses or Diagnosis

- Lifestyle history
- Medical history (such as Dementia or Alzheimer’s)
- Evaluation of blood and diagnostic tests
- Recommendations for testing (testing for allergies, for vitamin deficiencies)
- Evaluation of nutrition status (how serious is the deficiency)
- Calorie needs (based on height, weight, activity level, sex)
- Protein needs
- Nutrient needs
- Adequacy of your diet
- Possible diet deficiencies
- Food intolerance
The Takeaway…
Identifying malnutrition is an important first step in identifying a problem. Eating and enjoying a meal is part of our everyday life and important to everybody, not least to people living with dementia. A healthy diet and nutrition is fundamental to well being at any stage of life and to helping to combat other life-threatening diseases. Under nutrition is common among older people generally, particularly common among people with dementia. Under nutrition tends to be progressive, with weight loss often preceding the onset of dementia and then increasing in pace as the disease progresses. Although we can’t avoid these symptoms which lead to malnutrition and under nutrition, we can manage them with a variety of Nutrition Therapy Options. Orchard at Tucker’s 2018 Nutrition Therapy Program is designed to help combat under nutrition and bring back the joy of eating to those who have lost it. However it all starts with an nutrition assessment.




